Euthanasia & End of Life Issues
Learn
Though it is our top priority, Students for Life of America is not only working to stop abortion in our nation. We defend all innocent life from unnatural, systematic termination. Unfortunately, that means our work also includes euthanasia, an increasingly urgent problem in the United States.
Euthanasia is defined as the intentional taking of a person’s life, through direct action (called active euthanasia) or by inaction (called passive euthanasia), usually motivated by a "mercy" for those in great pain or suffering from a terminal illness [1]. However, the ends (stopping suffering) don’t justify the means (ending a life).
Both euthanasia and abortion are based on a view of people that lacks dignity. The pro-life movement views all life as precious and sacred, whether it is that of the elderly, the mentally ill, or preborn children. Pro-lifers recognize that life is an inalienable right, regardless of state recognition.
In contrast, those who call themselves “pro-choice” or “pro-assisted dying” view life as not inherently valuable but only as valuable as the worth assigned to it from a human source, such as the government. This worth may be based on any number of arbitrary factors, such as “quality of life,” etc. Such a worldview means that you must be human plus something else in order to be worthy of protection.
While there may be the best of intentions, it is blatantly discriminatory.
Voluntary Euthanasia
This is commonly known as “physician assisted suicide.” In such cases, the individual no longer wants to live and enlists the help of a medical professional in either killing them or allowing them to die (ceasing treatment, etc.). The most famous example of assisted suicide is that of Dr. Jack Kevorkian’s killing of 130 people, five of whom had no disease detected in autopsy [2]. Kevorkian served eight years in prison for second-degree murder. However, assisted suicide is now legal in ten states plus the District of Columbia.
Former Psychiatrist-in-Chief at Johns Hopkins Hospital, Dr. Paul McHugh, said, “With physician-assisted suicide, many people — some not terminally ill, but instead demoralized, depressed and bewildered — die before their time.” [3]
States where Assisted Suicide is Legal
- California
- Colorado
- District of Columbia
- Hawaii
- Maine
- Montana
- New Jersey
- New Mexico
- Oregon
- Vermont
- Washington State
You can find more information about state laws here.
Side Effects of Assisted Suicide Drugs
- The drugs used to commit suicide in these situations have disturbing side-effects that occur before the patient’s death.
- Barbiturates, a common drug used for assisted suicide, do not ensure a peaceful death. These are the drugs that are also used to kill criminals who have received the death penalty. Death by these drugs is regarded as cruel and unusual punishment — yet they are using them for assisted suicide.
- Overdoses of barbiturates are known to cause distress and have associated issues:
- Extreme gasping and muscle spasms
- While losing consciousness, a person can vomit and then inhale the vomit
- Panic, feelings of terror, and assaultive behavior from the drug-induced confusion
- Failure of drugs to induce unconsciousness
- A number of days elapsing before death occurs or death does not occur at all
Unfortunately, these issues with a “peaceful death with dignity” aren’t rare. A landmark data analysis found that complications occurred in 7% of PAS cases and problems of completion 16% of the time. This means something goes wrong nearly 1 in 4 times! [4]
Societal Harms
Assisted suicide not only takes life in an individual tragedy, but it also harms society. It confuses the role of a doctor and damages our medical culture. Rather than having confidence that a physician is there to treat and heal you, you may be worried that he/she will encourage suicide instead. Medical personnel have been caught on multiple occasions in the last decade making their own decisions about whether a patient should live or die.
In addition, consider psychiatrists. These are medical professionals who treat people every day with suicidal thinking and behavior. They should be trying to prevent their patients from killing themselves andtreating the underlying condition, not encouraging their patients to kill themselves.
If a physician may harm instead of heal, their entire mission is corrupted.
Beyond doctors, insurance companies or family members may also take wrongful advantage of assisted suicide due to it being perhaps the more inexpensive “way out.” For example, since 2008 in Oregon, medical systems have offered cancer patients assisted suicide instead of chemotherapy. Assisted suicide is cheaper than years of cancer treatment. There have been many cases where insurance offered to pay for the suicide pills but not for the life-saving treatment. These dangerous circumstances mean that a insurance company looking to save money or a family to preserve their inheritance may let their greed take someone’s life.
Involuntary Euthanasia
As involuntary mercy-killing is so obviously repugnant to most people, the most controversial form of euthanasia is called non-voluntary usually — that is, when the individual is not able to give or deny consent. The most famous examples are the cases of Terri Schiavo and Charlie Gard.
Terri Schiavo
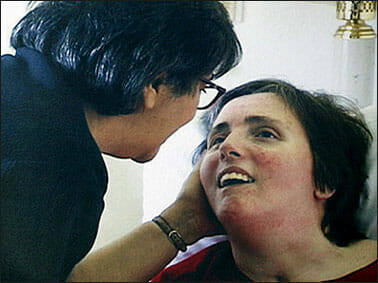
In 1990, at the age of 26, Terri Schindler Schiavo suffered a mysterious cardio-respiratory arrest. To this day, doctors have still not discovered a cause for this respiratory attack. She was diagnosed with hypoxic encephalopathy – neurological injury caused by lack of oxygen to the brain. She was placed on a ventilator.
Terri was soon able to breathe on her own and maintain vital function. She remained in a severely compromised neurological state (a persistent vegetative state [5]) and was provided a PEG tube to ensure the safe delivery of nourishment and hydration. Terri was kept alive by assisted feeding of food and water, the same things which keep us all alive [6].
In March 2005, Terri’s family fought a court order her husband had filed to pull her feeding and hydration tubes and kill her. For thirteen days, her family with the pro-life community battled the courts in vain. On March 31, 2005, Terri Schindler Schiavo died of marked dehydration following more than thirteen days without nutrition or hydration under the order of Circuit Court Judge George W. Greer of the Pinellas-Pasco’s Sixth Judicial Court. Terri was 41.
Charlie Gard

Another example of forced euthanasia happened in June 2017 in London. A 10-month-old baby named Charlie Gard was diagnosed with a rare genetic disease and hospitalized. His doctors decided that the best thing for Charlie was “death with dignity.” Charlie’s parents obviously disagreed with the doctors and searched for a doctor who would treat their baby. They found a doctor in the United States who agreed to treat Charlie and set up a Go Fund Me account to finance it.
They raised enough money (1.6 million) for Charlie’s trip to the U.S. and his treatment. However, the doctors prevented Charlie from leaving the hospital and told his parents that they were going to remove his life-support. His parents took it to the courts and the media, but after losing many court battles, the hospital switched off his life-support and said there was nothing that the parents could do. The hospital even refused his parents’ last wish: to take Charlie home. Charlie’s mom said, ‘We promised our little boy every single day that we would take him home’. Mr. Gard added: ‘We want to give him a bath at home, put him in a cot which he has never slept in, but we are now being denied that. We know what day our son is going to die but don’t get a say in how that will happen'[7]. Charlie passed away on July 28, 2017.
The United States is going down the same path. In Oregon, a 2018 law makes it legal to starve and dehydrate dementia and mentally-ill patients.
Videos:
More Resources
- Not Dead Yet
- Patient Rights Action
- The Family Institute of Connecticut
- The Heritage Foundation
- Euthanasia Facts
- Assisted Suicide: Frequently Asked Questions
- LifeIssues.net Euthanasia Library
- Medical Articles on Euthanasia
- PregnantPause on Euthanasia
- Terri Schiavo: Life & Hope Network
Definitions/Sources
[1] Traditionally defined as an illness or condition that will cause a person’s death within a relatively short time. Some state courts are expanding the term to include a condition in which death will occur if treatment, including nutrition and hydration, is removed.
[2] http://www.webcitation.org/5zijIM3U0
http://www.amednews.com/article/20110620/profession/306209944/4/
[4] https://www.nejm.org/doi/full/10.1056/NEJM200002243420805
[5] A condition in which the upper portions of the brain are damaged through disease or injury, but the brain stem is normal. Basic body functions such as breathing and digestion occur, and the individual has sleep-wake cycles. But these patients are not attentive, do not speak or have voluntary muscle movement.
[6] Nutrition that is provided with the help of another. This may be spoon-feeding, through a gastrotomy tube, or through a tube into the vein.
[7] https://www.dailywire.com/news/heartbreaking-parents-uk-baby-barred-potential-amanda-prestigiacomo

